 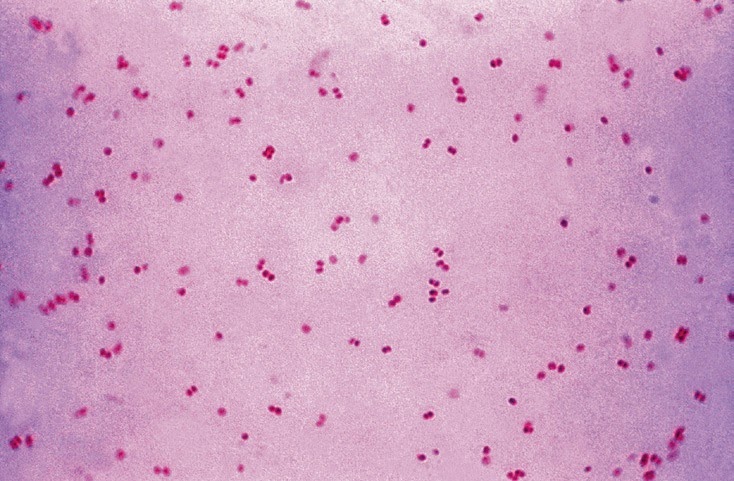
Septic arthritis caused by methicillin-resistant S. Large cohort study evaluating six weeks of therapy that was started within one week of surgery and/or treatment with intravenous antibiotics Oral antibiotics are not inferior to intravenous antibiotics for treatment of septic arthritis. Initial empiric antibiotic therapy for adults with septic arthritis should cover Staphylococcus aureus and Streptococcus species. 
4Įxpert opinion and consensus guideline in the absence of clinical trials Consideration for microorganisms such as Neisseria gonorrhoeae, Borrelia burgdorferi, and fungal infections should be based on history findings and laboratory results.īefore initiating antibiotic therapy in patients with suspected septic arthritis, analysis of synovial fluid obtained through arthrocentesis should be performed, including Gram stain, cultures, white blood cell count with differential, and crystal analysis. Total duration of therapy ranges from two to six weeks however, certain infections require longer courses. Oral antibiotics can be given in most cases because they are not inferior to intravenous therapy. After synovial fluid has been obtained, empiric antibiotic therapy should be initiated if there is clinical concern for septic arthritis. Staphylococcus aureus is the most common pathogen isolated in septic arthritis however, other bacteria, viruses, fungi, and mycobacterium can cause the disease. History and Gram stain aid in determining initial antibiotic selection. Synovial fluid studies are required to confirm the diagnosis. Physical examination findings and serum markers, including erythrocyte sedimentation rate and C-reactive protein, are helpful in the diagnosis but are nonspecific. A delay in diagnosis and treatment can result in permanent morbidity and mortality. Risk factors for septic arthritis include age older than 80 years, diabetes mellitus, rheumatoid arthritis, recent joint surgery, hip or knee prosthesis, skin infection, and immunosuppressive medication use. Users should refer to the original published version of the material for the full abstract.Septic arthritis must be considered and promptly diagnosed in any patient presenting with acute atraumatic joint pain, swelling, and fever. No warranty is given about the accuracy of the copy. However, users may print, download, or email articles for individual use. and its content may not be copied or emailed to multiple sites or posted to a listserv without the copyright holder's express written permission. Copyright of Journal of Intensive Care Medicine is the property of Sage Publications Inc.Further work is needed to determine the ideal time for critically ill adults to de-escalate from broad-spectrum antibiotics targeting Pseudomonas aeruginosa and extended-spectrum b-lactamase-producing gram-negative pathogens. Interpretation: Among a cohort of critically ill adults, 13% of respiratory cultures and 15% of blood cultures that ultimately grew GNRs resistant to ceftriaxone did not demonstrate growth until at least 48 hours after collection. Age, gender, predicted risk of inpatient mortality and prior use of antibiotics did not predict the growth of cultures after 48 hours. At 48 hours, 87% of respiratory cultures and 85% of blood cultures that ultimately grew GNRs resistant to ceftriaxone had demonstrated growth. A total of 376 blood cultures grew GNRs, of which 70 (18.6%) had resistance to ceftriaxone. Results: A total of 524 respiratory cultures had growth of GNRs, of which 284 (54.2%) had resistance to ceftriaxone. Multivariable logistic regression modeling was used to examine risk factors for the growth of cultures after 48 hours. 
The primary endpoint was the time-to-positivity of respiratory and blood cultures that ultimately demonstrated growth of GNRs resistant to ceftriaxone. Study Design and Methods: We conducted a secondary analysis of data from the Isotonic Solutions and Major Adverse Renal Events Trial: a pragmatic, cluster-randomized, multiple-crossover trial comparing balanced crystalloids versus saline for intravenous fluid administration in 15,802 critically ill adults at 5 intensive care units (ICUs) at Vanderbilt University Medical Center in Nashville, TN, USA. Research Question: We tested the hypothesis that cultures will identify GNRs that ultimately demonstrate resistance to ceftriaxone within 48 hours, potentially allowing safe de-escalation at this time point. Abstract: Background: The optimal timing for the de-escalation of broad-spectrum antibiotics with activity against Pseudomonas aeruginosa and resistant Gram-negative rods (GNRs) in critically ill adults remains unknown. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
